The immune system is a complex network of cells, tissues, and organs that work together to protect the body from foreign invaders, such as viruses and bacteria. This notes gives the details of cells of immune system.
The immune system is made up of several types of cells, each with a specific role in defending the body. These cells include white blood cells, also known as leukocytes, and antibodies, also known as immunoglobulins.
White blood cells are an essential part of the immune system, as they are responsible for detecting and attacking foreign invaders. There are several different types of white blood cells, including T cells, B cells, and natural killer cells.
T cells, also known as T lymphocytes, are a type of white blood cell that play a key role in cell-mediated immunity.
B cells, also known as B lymphocytes, are another type of white blood cell that is responsible for producing antibodies to help fight off infections.
Natural killer cells are a type of white blood cell that is able to attack and kill infected cells without the need for antibodies.

Antibodies, also known as immunoglobulins, are proteins produced by B cells that help to neutralise foreign invaders by attaching to them and marking them for destruction.
There are several different types of antibodies, including IgA, IgG, IgM, and IgE, each with a specific role in the immune response.
In addition to these cells, the immune system also includes tissues such as the spleen, lymph nodes, and bone marrow, as well as organs like the thymus and tonsils.
Together with the cells of the immune system, these tissues and organs give the body a full defence against foreign invaders.
Overall, the immune system’s cells are very important for keeping us healthy and keeping us from getting sick.
Understanding how these cells function and interact with each other can help us better understand how the immune system works and how we can support its function.
Lymphocytes are the immune system’s central cells, responsible for acquired immunity as well as the immunologic characteristics of diversity, specificity, many, and self- or non-self recognition. It constitutes 20% to 40% of the body’s WBC and 99% of the cells in the lymph.
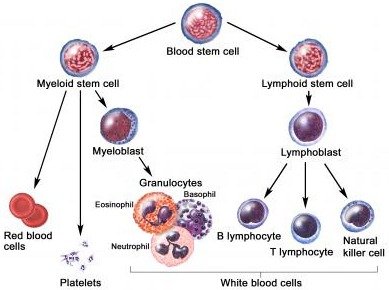
What are the Cells of the Immune system?
The basic cells of the immune system are lymphocytes (B- and T-cells), mast cells, granulocytes, and NK cells. These are basic immune cells.
B-Lymphocytes (B-Cells)
- The letter “B” designate from its site of maturation, in the “Bursa of Fabricius” in the birds; and “Bone marrow” in the mammalian species, including humans & mice.
- B-Lymphocytes carries out “Humoral-immune response” by producing antibodies.
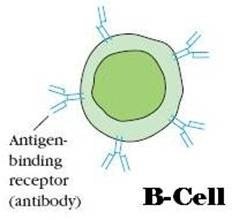
- B-Lymphocytes is stimulated by “Th -lymphocytes”.
- When the antigen stimulates, the B-cell divides repeatedly & differentiate over a 4 to 5 day period, generating a population of plasma cells & memory cells.
- Plasma cells lack membrane-bound antibody, synthesize and secrete one of the five classes of antibody.
- Each of the approximately 1.5X105 molecules of antibody on the membrane of a single B- cell has an identical binding site for antigen.
Development of B-Lymphocytes
B-cell differentiation, as assessed by membrane immunoglobulin expression, can be divided into antigen-independent and antigen-dependent phases. The bone marrow’s surrounding microenvironment influences antigen-independent differentiation of B cells: B-cells develop “clonal diversity” in the absence of antibody receptors for antigens.
B-cell development moves through several stages marked by the rearrangement of immunoglobulin genes. “Bone marrow stromal cells” influence all of these stages in two ways: 1) by direct contact with the stromal cells with B-cell precursors in the early stages of B-cell development and 2) by stromal cell-derived growth factors in the later stages of B-cell development.
Progenitor B-cells use their molecules to bind to stromal cells made of “Hyaluronic acid.” This activity promotes “C-kit ligand” (Stem Cell Factor) binding to C-kit-encoded “Tyrosine Kinase” membrane receptors.
Focus point: Once stimulated by antigen, the B cells lose IgD immunoglobulins. A percentage of the cells mature into memory cells. The B-cells then change into plasma cells, which make the immunoglobulins that are no longer on their surface.
T-Lymphocytes (T-Cells)
They are:
A. T-Helper cells (TH-Cells)
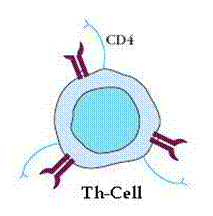
- The TH-cells recognize and bind to the combination of the antigen with the class -II MHC on the macrophage surface.
- TH-cells produce a variety of soluble factors known as “Cytokines“. The cytokines induce gamma-interferon” and other Macrophage activating factors“.
- The cytokines restore the microbicidal mechanism of the macrophage and bring about the death of the intracellular microorganisms.
B. Cytotoxic T-Cells (Tc -Cells)
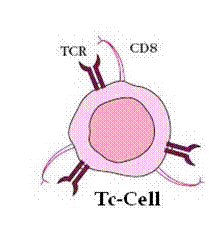
- The cells clonally express a large number of different surface receptors.
- Each Tc recognizes antigen only association with a cell marker, the class-l MHC.
- Tc also releases gamma-interferon.
- The cells recognize virally infected cells, which are killed before the virus replicates.
- Like B-cells, Tc – cells require help from Th-cells.
- These cells attack infected cells and cancer cells.
- The cells discharge a protein called “Perforin“, which lyses the infected cell.
c. T-Suppressor cells (Ts-cells)
T-cell receptor:
- The T-cell receptor was elucidated through the powerful recombinant DMA technology.
- The T-cell receptor called “Ti” (which is made up of two non-identical polypeptides- α & β chains and joined by a disulfide bond).
- The Ti associated with another protein called “CD3”.
Ti +CD3 –> Ti-CD3 complex
(T-cell receptor complex)

After many years, the immunologists identified the second type of receptor composed of gamma and 6-chains.
- The CDs are made up of at least three polypeptide chains (γ,δ, and Є).
Development of T-lymphocytes:
The T lymphocytes are derived from “hematopoietic stem cells” of the bone marrow. Some of these cells turn into “lymphopoietic progenitors.” The lymphoid progenitor cells turn into “pre-T-lymphocytes.” The pre-T cells leave the bone marrow and enter the thymus. In the thymus, they mature into T lymphocytes under the influence of thymic hormones. Mature T lymphocytes enter the bloodstream and colonize secondary lymphoid organs like the spleen, lymph nodes, Peyer’s patches, and so on. When exposed to antigens, they become functional.

Macrophages
- Macrophages are phagocytic cells, derived from the blood monocyte.
- Macrophages are part of the innate immunity.
- Macrophages are the general antigen-presenting cells.
- The Macrophages are amoeboid cells and having nucleus & prominent cytoplasmic lysosomes.
- Macrophages are very important cells of immune system.
- Macrophages like cells serve different functions in different tissues & are named according to their tissue location.
- Mononuclear phagocytic cell – monocyte circulating in the blood up to 8 hours, during which time they enlarge; they then migrate into the tissues & differentiate into specific tissue Macrophages and “ϒ-interferon”(ϒ-IFN) secreted by activated TH-cells.
Macrophages antimicrobial and cytotoxic activities:
Antimicrobial! & cytotoxic substances produced by activated macrophages can destroy phagocytosed microorganisms.
Mediators of antimicrobial and cytotoxic activity of macrophages and neutrophils
1. Reactive oxygen intermediates
- O2.- (Superoxide anion)
- OH– (Hydroxide radicals)
- H2O2 (Hydrogen peroxide)
- ClO– (Hypochlorite anion)
2. Reactive nitrogen intermediates
- NO (nitric oxide)
- NO2 (nitrogen dioxide)
- HNO2 (nitrous oxide)
3. Others
- NH2Cl (mono-chloramine)
Oxygen-independent killing
- Defensins
- Tumor necrosis factor-alpha
- (macrophage only)
- Lysozyme
- Hydrolytic enzymes
A) Oxygen-dependent killing mechanism
- Activated phagocytes produce a number of “Reactive Oxygen Intermediates (ROIs)” & “Reactive Nitrogen Intermediates” that have potent antimicrobial activity.
- During phagocytosis, a metabolic process known as the “Respiratory Burst” occurs in activated macrophages.
- Due to the respiratory burst, membrane-bound enzyme “Oxidase” will activate, that catalyzes the reduction of oxygen to superoxide anion (powerful oxidizing agent), a reactive oxygen intermediate & hydroxyl radicals &H2O
- As the lysosomes fuse with the phagosomes, the activity of “Myeloperoxidase” produces hypochlorite from hydrogen peroxide and chloride ions.
- Hypochlorite, the active agent of household bleach, is toxic to ingested microbes.
- When the macrophages are activated with bacterial cell wall components. The T-cell-derived cytokine (IFN-γ), they begin to express high levels of “Nitric Oxide synthetase“(NOS), an enzyme that oxidizes L-arginine to yield L-Citrulline & nitric oxide (NO), a gas.
- No has potent antimicrobial activity.
B) Oxygen-independent killing mechanism
- Activated macrophages also synthesize ‘lysozyme’ and various hydrolytic enzymes whose degradative activities do not require Oxygen.
- The activated macrophages produce a group of antimicrobials cytotoxic peptides, commonly known as “Defensin“, these Molecules are cysteine-rich cationic peptides containing 29-35 Amino acids residues.
- The defensin is circularized protein.
- The peptide form ion-permeable channels in the bacterial cell membrane.
Intracellular pathogens:
- Some microorganism can survive & multiply within pathogens include:
- Some intracellular pathogens prevent the fusion of lysosomes with phagosomes and proliferate within phagosomes.
What are Granulocytes?
Granulocytic cells
Granulocytes are a type of White Blood cells. These cells are considered body soldiers. The granulocytes are classified as neutrophils, eosinophils, and basophils on the basis of cellular morphology and cytoplasmic staining characteristics.
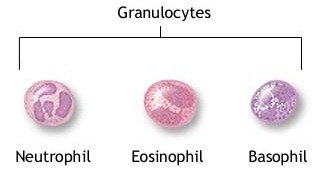
A. Neutrophils
It has a multilobed nucleus & granulated cytoplasm that stains with both acid & basic dyes.
- It is often called a “Polymorphonuclear leukocyte”(PMN)
- These are produced by hematopoiesis in the bone marrow, which is released into the tissues, where they have a lifespan of only a few days.
- Movement of circulating neutrophils into tissues called “Extravasation“.
- The neutrophils contain Primary & Secondary granules:
- Larger, denser primary granules: Peroxidase, Lysozyme, Various hydrolytic enzymes
- Smaller, secondary granules: Collagenase, Lactoferrin & Lysozyme
- Both primary & secondary granules are fuse with phagosomes.
- The cells exhibit a larger “Respiratory Burst” than macrophages & express higher levels of “defensins” than macrophages do.
B. Eosinophils
- The cells are motile phagocytic cells that can migrate from the blood into the tissue spaces.
- It has a bilobes nucleus & a granulated cytoplasm that stains with the acid dye “Eosin” red (hence its name).
- Play a significant role like a phagocytic role like macrophages.
- The secreted contents of eosinophilic granules may damage the parasite membrane.
C. Basophils
- It has a lobed nucleus and heavily granulated cytoplasm that stains with the basic dye “Methylene Blue“.
- These are non-phagocytic granulocytes, which release pharmacologically active substances from their cytoplasmic granules.
- These substances play a major role in certain “Allergic responses“.
Mast Cells
- These cell precursors are formed in the bone marrow by hematopoiesis.
- These are found in a wide variety of tissues, including the skin. Connective tissues of various organs, the
- Connective tissues of various organs, the Mucosal epithelial tissue of respiratory, Genitourinary & digestive tracts.
- These cells have a large number of cytoplasmic granules that contain “Histamine” and other pharmacologically active Substances.
- It plays an important role in the development of allergies.
Mast Cells Role in diseased conditions
A. Allergic disease
- Mast cells are a key part of asthma, eczema, itching (from different causes), allergic rhinitis, and allergic conjunctivitis. They also play a key role in allergic rhinitis and allergic conjunctivitis.
- Antihistamine drugs act by blocking the action of histamine on nerve endings.
- Cromoglicate-based drugs (sodium cromoglycate, nedocromil) block a calcium channel essential for mast cell degranulation, stabilising the cell and preventing the release of histamine and related mediators.
- Leukotriene antagonists, like montelukast and zafirlukast, stop leukotriene mediators from doing their job. They are used more and more to treat allergic diseases.
B. Anaphylaxis
In anaphylaxis, which is a severe systemic reaction to allergens like nuts, bee stings, or drugs, mast cells all over the body release their granules. This causes the blood vessels to widen and, if it’s bad enough, shock symptoms that could kill the person.
C. Autoimmunity
Mast cells are linked to the pathology of rheumatoid arthritis, bullous pemphigoid, and multiple sclerosis, all of which are autoimmune diseases. They have been shown to be involved in the recruitment of inflammatory cells to the joints (e.g., rheumatoid arthritis) and skin (e.g., bullous pemphigoid), and this activity is dependent on antibodies and complement components.
D. Reproductive disorders
Mast cells are found in the endometrium. In endometriosis, these cells become more active and release more mediators. Mast cells are found in the testes of males and are more common in oligo- and azoospermia. Mast cell mediators can directly stop sperm movement in a way that might be reversible.
E. Mast cell disorders
Mastocytosis is a rare condition featuring the proliferation of mast cells. It can affect the skin or spread to other organs. The skin-only form is called cutaneous, while the systemic form affects many organs. Mast cell tumors are often seen in dogs and cats.
Null Cells
- Null cells are lymphocytes with cytotoxic properties.
- They are neither B-cells or T cells. They are intermediate between T and B cells.
- They form less than 3%.
- There are two types of Null cells namely, Natural Killer Cells (NK cells) and Killer Cells.
A. Natural Killer Cells
- NK cells are a group of null cells.
- They form the third population of lymphocytes.
- The NK cells have 2 or 3 large granules in the cytoplasm. Hence they are also Large Granular Lymphocytes (LGL).
- They have a kidney-shaped nucleus.
- The NK cells kill the target cells without the aid of an antibody or complement. So they are antibody-independent.
- They destroy the cancer cells and cells infected with herpes and mumps virus.
- They are activated by Interferons and Interleukins-2.
B. Killer Cells (K cells)
- Killer cells are antibody-dependent.
- These cells possess Fc receptors for binding with IgG antibodies. Hence they can bind with cells coated with IgG antibodies and can kill them.
- These cells can combine with a specific antibody when it is in a complex with antigen. If the complex is on the surface of a target cell, these lymphocytes become activated destroying the target cell.
- This cell can kill a variety of cells such as tumor cells, bacteria, viruses, fungi, and parasites.
Final words on Immune cells
The immune system is a complex network of cells, tissues, and organs that work together to protect the body from foreign invaders. This article explores the different types of cells that make up the immune system, including white blood cells and antibodies, and how they work together to keep us healthy.
Learn about the role of T cells, B cells, natural killer cells, and various types of antibodies in the immune response, and how the tissues and organs of the immune system support their function.